Australia is a hard country with massive droughts, massive rainfalls every 10 years (like now) and quite weird behavior.
Stories like the following appear daily. The weird ones.
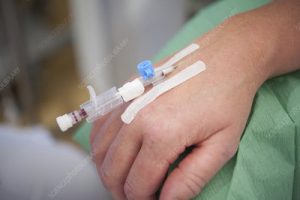 Heath Parkes-Hupton of The Australian writes a mum accused of putting feces in her son’s cannula as he writhed in pain at a Sydney hospital was heard being asked by her sick child “why are you doing this to me”, a court has heard.
Heath Parkes-Hupton of The Australian writes a mum accused of putting feces in her son’s cannula as he writhed in pain at a Sydney hospital was heard being asked by her sick child “why are you doing this to me”, a court has heard.
The boy’s mother is facing a special hearing at Downing Centre District Court for allegedly poisoning her then nine-year-old son through his cannula while he was a patient at The Children’s Hospital at Westmead in September 2014.
The woman, a mother of four who can’t be named, denies infecting the boy and has pleaded not guilty to using poison to endanger a life.
His blood culture later tested positive to the bacteria E. coli.
The mother’s barrister Pauline David told the court on Thursday there were a number of possibilities that could explain how the boy became infected.
Crown witness and nurse Lindie Brown, who was working at a unit manager at the ward where the boy was a patient, told the court he became “very unwell” during one of her shifts.
The court heard the boy had a temperature of 40C and began experiencing rigors – or shaking.
He was also complaining of pains in his back, stomach and head and asked for medicine to “take the pain away”, the court heard.
Ms Brown told the court she then heard the boy ask his mother “why she was doing this to him”.
He then said words to the effect of “you could have put something in my cannula when I was asleep”, Ms Brown said.
The hearing before Judge Justin Smith continues.













